New method for assessing response to neoadjuvant chemotherapy for esophageal cancer
Will lead to more accurate prediction of long-term survival and development of treatment strategies based on metabolic tumor volume
Osaka University researchers demonstrated that it was possible to more accurately evaluate responses to preoperative chemotherapy, or neoadjuvant chemotherapy (NACT), in patients with locally advanced esophageal cancer (EC) by assessing the activity of metabolic tumor volume (MTV) by 18 F -fluorodeoxyglucose-positron emission tomography/computed tomography ( 18 F -FDG PET/CT) before and after the preoperative chemotherapy series, standard treatment for EC.
For treating locally advanced EC, patients usually undergo NACT before surgery because surgery following NACT can reduce the risk of recurrence of cancer. Surgery after NACT is associated with a better prognosis in patients than NACT after surgery, even if the same type of surgery is conducted. Thus, it is important to accurately assess treatment response in order to predict long-time survival.
Usually, treatment response can be assessed by the reduction rate of tumors in surgical specimens. To provide patient-tailored treatment, it is necessary to predict treatment response by image diagnosis before surgery, but optimal methods to evaluate treatment response for EC patients have not yet been established.
The researchers focused on MTV change before and after chemotherapy, which is measured by 18 F -FDG PET/CT. In conventional therapeutic response assessment by computer tomography (CT) tumor measurements and general Maximum Standard Uptake Value (SUVmax), differences in long-term survival have not been fully clarified; however, the researchers demonstrated that a cut-off value of 60% MTV reduction (metabolic tumor volume change) was best in predicting treatment response.
Using multivariate analysis, they examined the most significant factor for the prediction of long-term survival from factors, such as gender, age, the progress of cancer, and response evaluation by CT, MTV, and SUVmax, demonstrating that the MTV reduction rate was the only factor to accurately predict long-term survival.
These results will greatly contribute to the establishment of patient-tailored therapy; that is, it will become possible to provide patient-tailored chemotherapy and radiation therapy to EC patients who did not respond to standard chemotherapy, which will lead to the improvement of treatment outcomes of locally advanced EC, EC in general, and eventually various cancers other than EC.
Abstract
Objective: Here, we assess the ability of metabolic tumor volume (MTV) as measured by 18 F-fluorodeoxyglucose-positron emission tomography/computed tomography ( 18 F-FDG PET/CT) to evaluate neoadjuvant chemotherapy response for patients with locally advanced esophageal cancer (EC).
Background : Optimal methods to evaluate treatment response for EC patients have not yet been established. Although previous studies have reported the value of standardized uptake value (SUV), the accuracy of predicting histological response or long-term survival in EC is limited.
Methods : In all, 102 EC patients without distant metastasis who underwent 18 F-FDG PET/CT both before and after the preoperative chemotherapy series were analyzed.
Results : The median primary tumor MTV values before and after preoperative chemotherapy were 22.55 (range 0.4–183.1) and 2.75 (0–52.9), respectively, and the median MVT reduction rate was 86.5%. We found the most significant difference in survival between PET responders and nonresponders with a cut-off value of 60% MTV reduction, using a 10% stepwise cut-off analysis [2-year progression-free survival (PFS): 79.2 vs 44.4%; hazard ratio (HR) 3.397; P < 0.0001). With this cut-off value, histological response (P = 0.0091), tumor location (P = 0.0102), pT (P = 0.0011), and pN (P = 0.0110) were significantly associated with PET response. Univariate analysis of PFS indicated a correlation between PFS and tumor size, cT, decrease of primary lesion by CT, SUVmax reduction rate, MTV reduction rate, pT, pN, and pM. Multivariate analysis further identified pM and MTV reduction rate to be independent prognostic predictors (HR 2.471; P = 0.0263), but not decrease of primary lesion by CT or SUVmax reduction rate (HR 3.063; P = 0.0279).
Conclusion : MTV change is clinically useful in predicting both long-term survival and histological response to preoperative chemotherapy in EC patients, after determining the optimal cut-off value based on survival analysis.
Figure 1. Possible algorism of a treatment strategy for advanced esophageal cancer; patients with > 60% decrease of MTV receive surgery right after chemotherapy while patients with < 60% decrease of MTV may be suitable for other type of chemotherapy or chemo-radiation followed by surgery to improve survival.
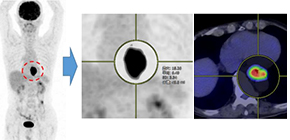
Figure 2. Measurement of MTV in FDG-PET; Performing PET-CT before and after preoperative chemotherapy for esophageal cancer, SUVmax and MTV were respectively measured by using volume viewer software, SYNAPSE VINCENT (Fujifilm Medical®, Tokyo, Japan).
Figure 3. Survival prediction by using PET parameters before and after preoperative chemotherapy for esophageal cancer; survival according to SUVmax (left, conventional PET parameter) and MTV (right). MTV enables more accurate prediction of patient survival compared with SUVmax.
The article, “Metabolic Tumor Volume Change Predicts Long-term Survival and Histological Response to Preoperative Chemotherapy in Locally Advanced Esophageal Cancer” was published in the Annals of Surgery at DOI: https://doi.org/10.1097/SLA.0000000000002808
Related links
