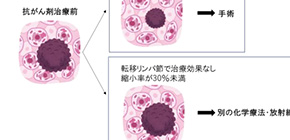
Lymph nodes can predict survival in patients with esophageal cancer
Researchers from Osaka University Graduate School of Medicine find that lymph nodes may be more useful than previously-used indicators for predicting recurrence and survival in patients with esophageal cancer
Optimal methods for predicting treatment efficacy in patients with esophageal cancer are seriously lacking. But now, researchers from Japan have found a useful alternative to existing methods for predicting patient outcomes.
In a study published this month in Annals of Surgery , researchers from Osaka University revealed that, compared with primary tumors, which are often used to assess treatment outcomes in many types of cancers, the response of lymph nodes to neoadjuvant chemotherapy (NACT) is more effective in predicting disease recurrence and patient survival in individuals with esophageal cancer.
Although imaging techniques such as computed tomography (CT) and endoscopy are often used to examine primary tumors in cancer patients, these techniques are not helpful when trying to measure primary tumors in the esophagus because of its shape. Thus, it is difficult for physicians to estimate recurrence and survival in patients with esophageal cancer. The research team attempted to address this issue by finding another indicator of patient outcome.
“The frequency of lymph node metastases are very high particularly in advanced esophageal cancer compared with other gastrointestinal cancers,” say lead authors Shinya Urakawa and Tomoki Makino. “Consequently, we reasoned that the response of lymph nodes might be more useful than that of primary tumors for predicting chemotherapeutic efficacy and patient prognosis. Accordingly, we aimed to determine the clinical utility of lymph node responses to NACT for predicting long-term survival in patients with metastatic esophageal cancer.”
To do this, the researchers used CT to measure metastatic lymph nodes before and after NACT in individuals with metastatic esophageal cancer. They evaluated the chemotherapeutic response by monitoring the respective sizes of primary tumors and all metastatic lymph nodes that met a specific set of criteria.
“CT scans conducted before and after NACT demonstrated a high discordance in the response between primary tumors and metastatic lymph nodes in patients with esophageal cancer,” explains Yuichiro Doki.
In fact, the researchers found that every lymph node showed a different response, even those in the same patient. Thus, it might be helpful to consider all metastatic lymph nodes to obtain a precise assessment of the NACT response.
“The lymph node response facilitated precise predictions of patient prognosis,” says Urakawa and Makino. In addition to facilitating outcome predictions, this finding could contribute to the optimization of treatment strategies, and eventually lead to improved survival in patients with metastatic esophageal cancer.

Figure 1. CT evaluation of response to neoadjuvant chemotherapy. The PT area was bi-dimensionally measured, based on the greatest diameter and the greatest perpendicular length (A). The LN response was evaluated by measuring the minor axes of all positive LNs, and the sum was calculated, based on RECIST (Response Evaluation Criteria in Solid Tumors) criteria (B).

Figure 2. Recurrence-free survival among NACT responders and nonresponders. (A) PT response, (B) LN response. PT-R: PT-responders; PT-NR: PT-nonresponders; LN-R: LN-responders; LN-NR: LN-nonresponders

Figure 3. Comparison of recurrence among NACT responders and nonresponders. 5-year cumulative rates of (A) lymphatic recurrence, (B) hematogenous recurrence.
The article, “Lymph node response to neoadjuvant chemotherapy as an independent prognostic factor in metastatic esophageal cancer,” was published in Annals of Surgery at DOI: https://doi.org/10.1097/SLA.0000000000003445 .
Related links
