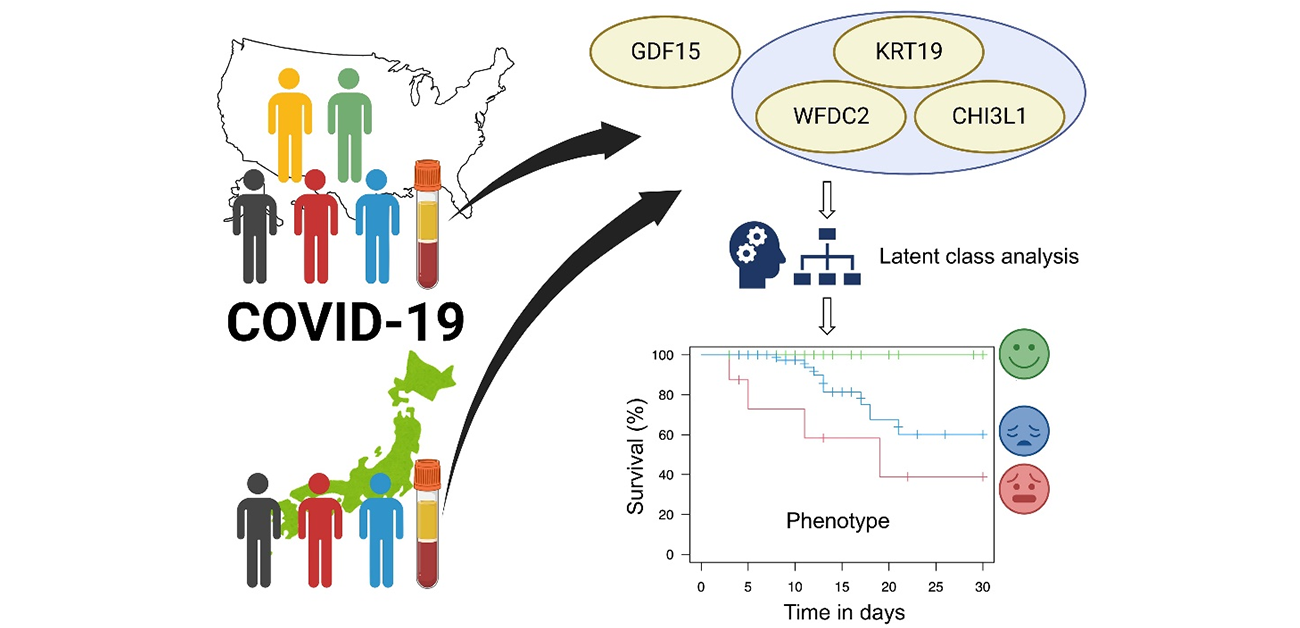
Investigating the plasma to predict COVID-19 progression
Researchers led by Osaka University used an innovative proteomics method to identify four proteins in the blood that are associated with critical pathogenesis in patients with COVID-19
Just as oil is essential to keep a car’s motor running, blood is essential to keep the body functioning. The presence of particular proteins in the plasma, the liquid component of blood, may signal the presence of a disease or indicate the severity of a condition. Now, researchers in Japan have uncovered several key plasma proteins that are related to severe COVID-19.
In a new study published in Journal of Clinical Immunology, a research team led by Osaka University used a novel blood screening method to analyze proteins in plasma samples from two large patient cohorts and identified five proteins associated with the development of severe COVID-19.
COVID-19 is associated with inflammation, and excessive inflammation may lead to organ failure. One method to assess inflammation in the body is to evaluate proteins circulating in the blood plasma. The team set out to identify specific plasma proteins that may reflect the severity of COVID-19 infection and thus may potentially be used to identify patients with COVID-19 who are at risk for poor outcomes. To conduct the investigation, the team evaluated datasets from American and Japanese cohorts that included patients with critical COVID-19, those with non-critical COVID-19, and healthy volunteers.
“We began by analyzing publicly available blood data from the US cohort to determine candidate plasma proteins that are differentially expressed in critical and non-critical COVID-19 cases,” says lead author Takeshi Ebihara.
The plasma proteins were measured by an innovative blood analysis method, Olink proteomics and the researcher identified 28 candidate proteins in the American cohort. Evaluation of these candidate proteins in the Japanese cohort narrowed the candidate proteins down to five plasma proteins that were more highly expressed in severe COVID-19 patients than in healthy controls.
The researchers then used an immunoassay technique to evaluate expression of these five candidate proteins in a validation cohort which was composed of Japanese patients with severe COVID-19. Levels of four of the candidate proteins, WFDC2, GDF15, CHI3L1, and KRT19, were significantly higher in COVID-19 patients compared with healthy controls and were more frequently elevated in non-survivors than in survivors.
“Our results showed that these four proteins appear to be linked to COVID-19 severity,” says lead author Takeshi Ebihara. “Interestingly, the proteins are all related to cell adhesion pathways, which suggests that their role in the pathogenesis of severe COVID-19 could come from the dysregulation of these pathways.”
The identified proteins may have the potential to serve as biomarkers to predict prognosis in patients with COVID-19. In the future, rapid diagnostic kits to identify patients at risk of severe COVID-19 are expected to be applied in the clinic. Additionally, the proteins may represent potential targets for the development of therapies for the treatment COVID-19.
Fig.
Graphic abstract
License: CC BY4.0
Credit: 2022, Takeshi Ebihara, Combination of WFDC2, CHI3L1 and KRT19 in plasma defines a clinically useful molecular phenotype associated with prognosis in critically ill COVID 19 patients, Journal of Clinical Immunology
The article, “Combination of WFDC2, CHI3L1, and KRT19 in Plasma Defines
a Clinically Useful Molecular Phenotype Associated with Prognosis in Critically Ill COVID‐19 Patients,” was published in Journal of Clinical Immunology at DOI: https://doi.org/10.1007/s10875-022-01386-3.
Related links
