Effectiveness of L-P Shunt for idiopathic normal pressure hydrocephalus patients verified
Idiopathic normal pressure hydrocephalus develops in the elderly, causing symptoms such as gait disorder, dementia, and involuntary urination due to liquid accumulated in the brain. A group of researchers at Osaka University, Tohoku University, Juntendo University, and Rakuwakai Healthcare System verified the effectiveness of lumboperitoneal shunt (L-P Shunt) placement in idiopathic normal pressure hydrocephalus in multicenter trials in collaboration with 20 institutes in Japan, a world first.
- Graduate School of Medicine, Osaka University -- KAZUI Hiroaki , Lecturer
- Graduate School of Medicine, Tohoku University -- MORI Etsuro , Professor
- Faculty of Medicine, Juntendo University -- MIYAJIMA Masakazu , Associate Professor
- Normal Pressure Hydrocephalus Center, Rakuwakai Healthcare System -- ISHIKAWA Masatsune
In the past, ventriculoperitoneal shunting (L-P Shunt) was mainly used for treating idiopathic normal pressure hydrocephalus; however, a shunt tube was inserted into the brain so there was a possibility to cause brain damage. This group's treatment did not damage the brain, demonstrating the effectiveness of L-P Shunt.
Abstract
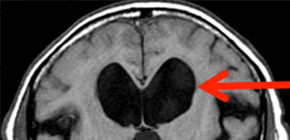
Cerebrospinal fluid (CSF) surrounds the brain and spinal cord. It is produced by the choroid plexus in the ventricles of the brain, circulates around the brain moving from ventricle to ventricle, and is absorbed into the venous circulation and lymphatic vessels (Figure 1, left). Hydrocephalus is a condition in which there is too much CSF in the ventricles. Idiopathic normal pressure hydrocephalus (iNPH) is a type of hydrocephalus and occurs when the natural system for draining and absorbing extra CSF does not work right. In iNPH, the ventricles enlarge to accommodate the extra fluid (Figure 1, right) and then press on different parts of the brain, causing a number of different symptoms, including gait disturbance, cognitive impairment, and urinary incontinence (triad symptoms) (Figure 2). Recent epidemiological studies conducted in Japan disclosed that iNPH is a common disease with a prevalence of 1.1% in Japanese elderly community residents. Although iNPH is considered to be treatable with CSF shunts, there is no high-level evidence indicating that CSF shunts are beneficial for iNPH.
SINPHONI (Study of Idiopathic Normal Pressure on Neurological Improvement: SINPHONI)-2 was a project of the Japanese Society of Normal Pressure Hydrocephalus and a multicentre prospective trial of lumbo-peritoneal shunt surgery, in which CSF is redirected from the lumbar spinal subarachnoid space to the abdominal cavity (Figure 3), for iNPH patients. Ventriculo-peritoneal shunt surgery, in which CSF is redirected from the lateral ventricle to the abdominal cavity, is the most commonly used treatment approach for this disease in other countries than Japan. However, more patients with iNPH were treated by lumbo-peritoneal than by ventriculo-peritoneal shunt surgery in Japan in 2011, which can be attributed to the fact that ventricular catheter placement is associated with a roughly 1% risk of symptomatic intraparenchymal haematoma and because, in our experience, patients are more willing to accept lumbar surgery than cranial surgery. Ninety three iNPH patients were recruited from 20 neurological or neurosurgical centres in Japan between March 1, 2010 and October 19, 2011 in SINPHONI-2. The subjects were randomly assigned to either the immediate group (n=49), who received lumbo-peritoneal shunt surgery immediately after the randomisation, or the postponed group (n=44), in whom the surgery was postponed for three months. All subjects were instructed to do physical exercises during the study period. The primary endpoint and main secondary endpoint were defined as favorable outcome (an improvement of one or more points on the modified Rankin scale, which is a scale for measuring the degree of disability or dependence in the daily activities) at three months after the randomization, and 12 months after the surgery, respectively.
The patients who reached the primary endpoint were significantly greater in the immediate group (32 of 49 patients (65%)) than the postponed group (2 of 44 patients (5%)) (p<0.0001, Fisher’s exact test) at three months after the randomization (Figure 4). The triad symptoms improved significantly in the immediate group but did not improved significantly in the postponed group at three months after the randomization. These results show that lumbo-peritoneal shunt surgery is effective for iNPH patients. The patients those who reached the main secondary endpoint were comparable between the two groups (immediate: 30 of 45 patients (67%), postponed: 22 of 38 patients (58%)) (p=0.496, Fisher’s exact test) at 12 months after the surgery. Severe adverse events that were related to shunt placement were reported in 10 patients (11%): subdural haematoma requiring surgery in 3 patients, shunt tube migration requiring surgical repair in 5 patients, shunt tube rupture requiring revision in 1 patient and meningitis in 1 patient. The present study is the first randomized controlled trial to show that patients with iNPH benefit from shunt surgery in terms of functional status and triad symptoms. It is also the first to show the efficacy of lumbo-peritoneal shunt surgery in patients with iNPH.
This investigator-initiated study was supported in part by Johnson & Johnson K.K. and Nihon Medi-Physics Co. Ltd.
Figure 1: Circulation of CSF in the brain (left) and enlargement of ventricles in patients with iNPH (right)
Figure 2: Triad symptoms of iNPH
Gait disturbance, cognitive impairment, and urinary incontinence are the triad symptoms of iNPH. The triad symptoms interfere with everyday activities of iNPH patients.
Figure 3: Two kinds of shunt surgery for iNPH patients
Left: lumbo-peritoneal shunt surgery
CSF is redirected from the lumbar spinal subarachnoid space to the abdominal cavity.
This shunt surgery was used in the present study and could avoid puncture-induced damage to the brain associated with ventricular shunt surgery.
Right: ventriculo-peritoneal shunt surgery
CSF is redirected from the lateral ventricle to the abdominal cavity.
This surgery is the most commonly used treatment approach for iNPH in other countries than Japan.
Figure 4: Effect of lumbo-peritoneal shunt surgery for iNPH patients
The subjects in this study were randomly assigned to either the immediate group, who received lumbo-peritoneal shunt surgery immediately after the randomisation, or the postponed group, in whom the surgery was postponed for three months. The assessments were conducted 3 months after the randomization and 12 months after the lumbo-peritoneal shunt surgery.
Left: The patients who showed an improvement of one or more points on the modified Rankin scale were significantly greater in the immediate group (32 of 49 patients (65%)) than the postponed group (2 of 44 patients (5%)) (p<0.0001, Fisher’s exact test) at three months after the randomization.
Right: The patients who showed an improvement of one or more points on the modified Rankin scale were comparable between the two groups (immediate: 30 of 45 patients (67%), postponed: 22 of 38 patients (58%)) (p=0.496, Fisher’s exact test) at 12 months after the surgery.
To learn more about this research, please view the full research report entitled " Lumboperitoneal shunt surgery for idiopathic normal pressure hydrocephalus (SINPHONI-2): an open-label randomised trial " at this page of the Lancet Neurology website .
Related Link
