Getting things under control: new mouse model aids study of immunomodulation
Osaka University-led research team has generated a novel mouse model to study complex mechanisms of immunomodulatory human disease therapies that are ineffective in wild-type mice
Because mice do not respond to immunomodulatory drugs (IMiDs), preclinical therapeutic and safety studies of the effects of IMiDs have not been possible in existing types of mice. This has led to an inability to accurately assess the mechanism of these drugs in mice. This in turn has led to several notable worldwide medical scandals, such as the one involving thalidomide in the late 1950s and early 1960s, wherein thousands of children suffered birth deformities not indicated in the tested mice. Since then, many studies have attempted to understand and overcome this limitation in assessment of IMiDs; none have been successful, until now.
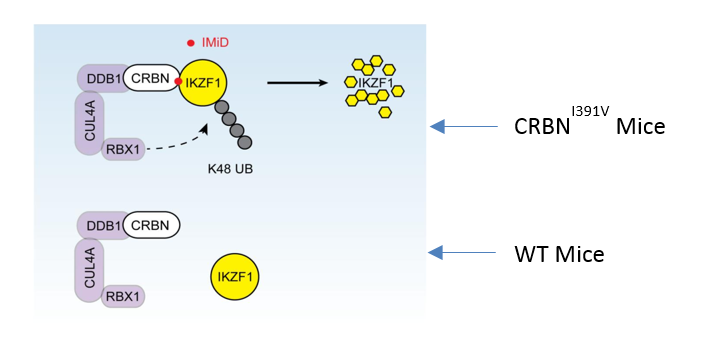
In a new study published in the Proceedings of the National Academy of Sciences of the United States of America (PNAS) , a research team led by experts from Osaka University generated a new type of mouse with a humanized cereblon receptor, which is the primary protein that interacts with IMiDs, and found that these new mice respond to IMiD treatment.
“In our study, we found that treatment with a novel IMiD resulted in a degradation of Cullin4A/B CRBN E3 ligase substrates that involves in various cellular regulations, some of which are a transcription factors that regulates T and B cells,” says the corresponding author Tadamitsu Kishimoto. “Moreover, this new IMiD upregulates IL-2 production in a CRBN-IMiD binding region dependent pathway, which may further aid in the regulation of T cell activity.”
The researchers used dextran sodium sulfate to induce colitis in the new mice and in wild-type mice to test the therapeutic effects of IMiDs in colitis. The results suggested that IMiDs had similar effects in both types of 1mice.
“Our analyses revealed that lenalidomide and pomalidomide, two IMiDs used for cancer treatment provide an anti-colitis therapeutic benefit,” says lead author Yohannes Gemechu. “This benefit is mediated through a pathway that is independent of Cereblon-IMiD binding region, which suggests that our new mouse model may help to identify drugs that can be tested in wild-type mice.” He emphasized, “the study in wild type mice needs extra-caution because these mice are resistant to majority of toxic and therapeutic effects of IMiDs as opposed to our new mice.”
In addition to potentially enabling the study of a range of IMiDs in mice, this new model allows assessment of therapeutic effects of drugs that may be toxic to humans. If effective, these drugs could potentially be modified to a non-toxic form, thus providing new immunomodulatory therapies.
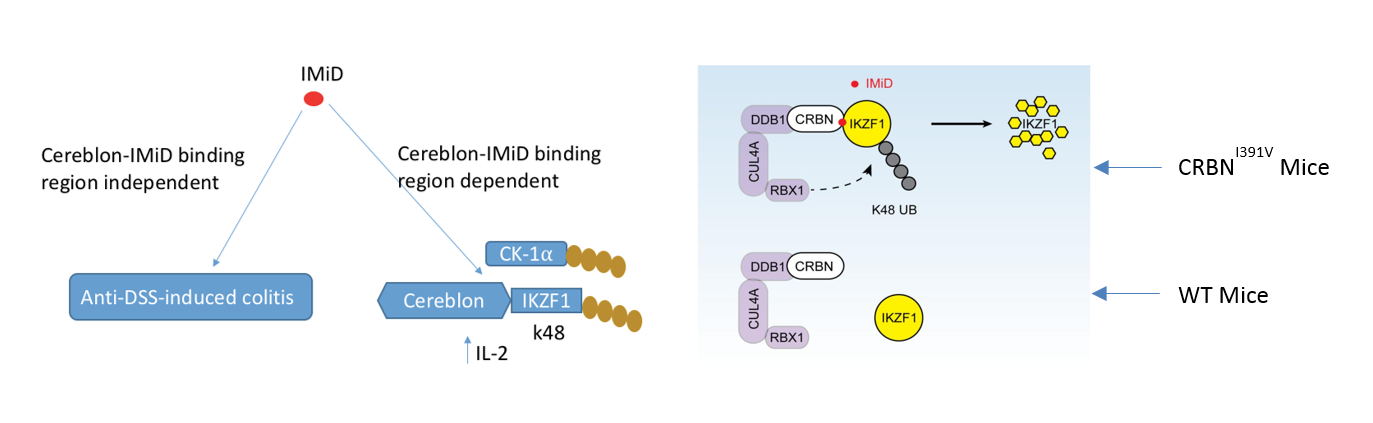
Figure : Two different pathways in a humanized cereblon mouse model.
Kishimoto and colleagues found that the degradative effect of IMiDs on IKZF1 and CK-1α, as well as upregulation of IL-2, is dependent on the CRBN-IMiD binding region. Therefore, the anti-inflammatory bowel disease benefit of IMiD is mediated through a CRBN–IMiD binding region-independent pathway. (credit: Osaka University)
The article, "Humanized cereblon mice revealed two distinct therapeutic pathways of immunomodulatory drugs," was published in PNAS at DOI: https://doi.org/10.1073/pnas.1814446115
Related links
